https://www.cdc.gov/pcd/issues/2021/21_0123.htm
A few days ago the CDC published findings detailing underlying medical conditions of hundreds of thousands of U.S. patients who were hospitalized with severe COVID-19 symptoms. The data was from the period of March, 2020 – March, 2021, from 800 hospitals, and included adults 18 years and older. Here’s a synopsis of the key findings:
- Of the 4.9M hospitalized adults, about 540K (11%) were hospitalized with COVID-19
- Of the 540K hospitalized, 94.9% of the patients had at least one underlying chronic health condition
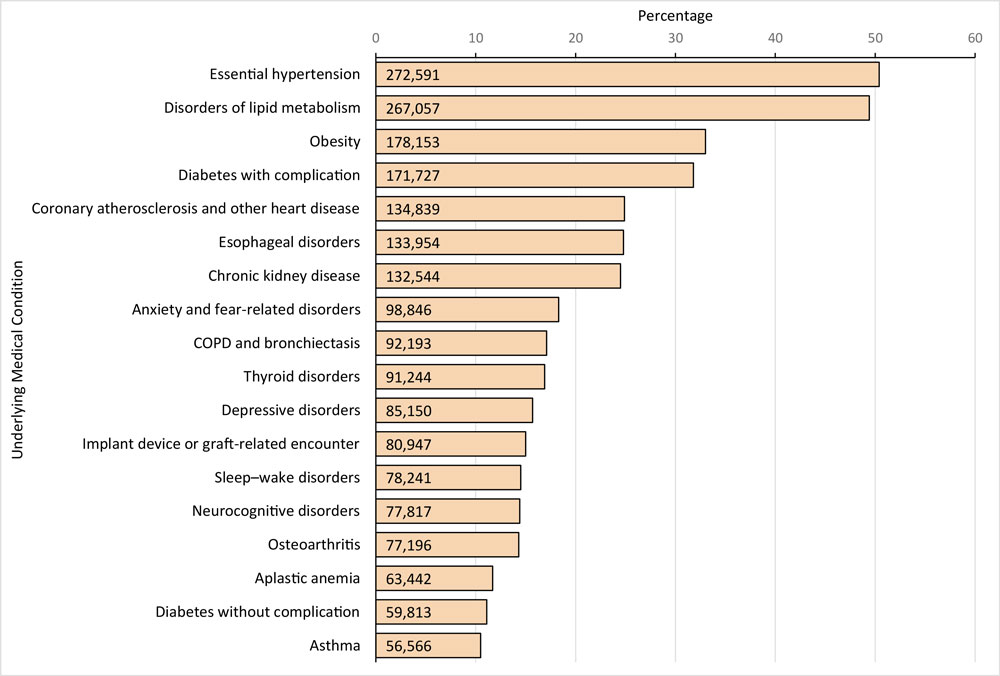
- The most common chronic conditions, or diseases, were:
- Hypertension, or high blood pressure (50.4%)
- Lipid Metabolism Disorder (49.4%)
- Obesity (33%)
- Note: The 4th and 5th diseases were diabetes and coronary atherosclerosis, or heart disease
- The highest risk factors for death from COVID-19 existed in patients with the following diseases:
- Obesity
- Anxiety and Fear Related Disorders
- Diabetes
Metabolic Syndrome
We’ve highlighted the linkage between obesity and COVID-19 in previous articles at http://www.business-fit.org, and this data only raises the sense of urgency around our dietary lifestyle and the health issues it can create. Obesity is linked to 8 out 10 of the leading causes of death in the U.S., but it also comes with perceptual issues that create animosity, embarrassment and anxiety in people who suffer from it. Obesity is so much more than just a simple, and outdated, adage of “calories-in vs. calories-out.” A better way to think about obesity is something called Metabolic Syndrome. Let me explain.
A syndrome is defined as “a set of medical signs and symptoms which are correlated with each other and often associated with a particular disease or disorder.” So, when we talk about metabolic syndrome, what we’re highlighting is a group of conditions that correlate around metabolic disfunction, and lead to serious conditions or diseases such as cardiovascular disease, stroke, type II diabetes, renal (kidney) disease, obesity, and others. Genetics, body types and hormonal issues all contribute to metabolic syndrome, and can be a key reason why two people in the same family have such a different physiology when it comes to, for example, obesity. By focusing on metabolic syndrome, we recognize there are several factors that could be contributing to a person’s poor metabolic health and not just assuming the person is unable to exhibit portion control. We can actually test to identify metabolic syndrome risk, and there are typically six core metrics used to measure whether someone either has, or is at risk of developing, metabolic syndrome. They are:
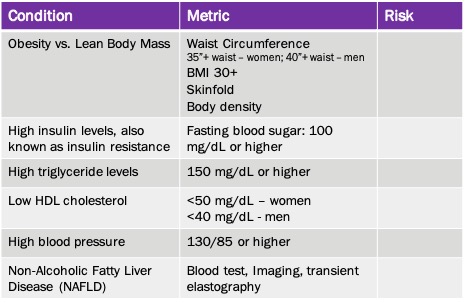
Put simply, these six conditions can be identified through various testing methodologies, and if a patient has three of these, they are certainly at risk for metabolic syndrome. More than three, and it’s pretty clear this patient has it, and is in very poor metabolic shape. A doctor, through this testing, can identify the risk level of a patient based on the ranges for each test, and then work with the patient to make dietary and lifestyle changes to reverse this syndrome.
Application to COVID-19
Referring back to the CDC data, we know diseases like cardiovascular (including high blood pressure), lipid metabolism, diabetes and obesity are all very clearly linked to severe COVID-19 symptoms, and even with a higher risk of death. As we assess vaccination levels, people who are at higher risk of severe symptoms vs. those that are at lower risk, and how to establish a health and wellness strategy that enables us to be proactive without placing onerous and damaging lockdowns on the entire population, we need to follow a two-pronged strategy:
- Metabolic Syndrome Prevention & Reversal. Proactive change is the key. If patients and doctors begin testing and monitoring these six areas consistently, metabolic syndrome can be identified earlier and corrected before it becomes high risk. Knowing which patients have metabolic syndrome can also enable a doctor to establish a closer monitor of such patients as it relates to COVID-19 risk. Even better, with good dietary and lifestyle advice, patients can avoid even becoming at risk for metabolic syndrome, which significantly lowers the risk of severe COVID-19 symptoms.
- Early Bridge Treatments for High Risk Patients. For those suffering from metabolic syndrome, course correction is paramount, and can be done without drugs in most cases. But again, it starts with testing and understanding, then an honest review of lifestyle behaviors and how to change. Because a change does not occur overnight, for these patients, there needs to be a near-term or “bridge” treatment that can be administered to keep COVID-19 from ravaging the body and causing the immunogenic and cytokine responses that lead to severe or even fatal conditions.
By applying focus, understanding the key conditions that drive COVID-19 severe symptoms and which patients are at high risk, ensuring a bridge treatment for those who do become sick with COVID-19 BEFORE it gets too serious, and establishing a prevention and reversal plan, we can change the trajectory of chronic disease while enabling a much better management and progression beyond a world being defined by COVID-19.
